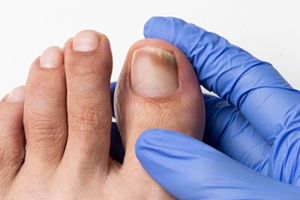
Causes and Prevention of Blisters From Running
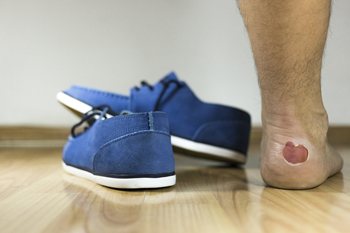
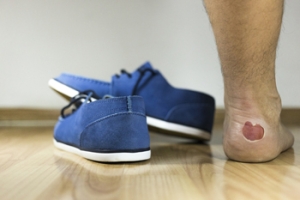
Blisters are common injuries for runners, often caused by friction between the skin and footwear or socks. When a runner's feet move within shoes that do not fit properly or are made of materials that rub against the skin, the skin layer becomes irritated, resulting in a fluid-filled bubble. Several factors contribute to blister formation, including moisture, prolonged pressure, and wearing poorly-fitting shoes. The friction intensifies with sweat, causing the skin to become more vulnerable. In addition to uncomfortable shoes, wearing socks made from cotton rather than moisture-wicking materials can increase the risk of blisters. To prevent blisters while running, it is important to choose well-fitting shoes and wear socks that keep feet dry. Taking care to check for any areas of irritation during runs can also help in preventing painful blisters. If you have a foot blister that is bothersome or has become painful, it is suggested that you consult a podiatrist who can offer effective relief and prevention methods.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Kenneth Donovan, DPM of Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters
Blisters are small pockets of fluid that occur on the top layers of the skin for several reasons. Friction, burns, and diseases are all known causes of blisters. Smaller blisters are known as vesicles, while larger blisters are referred to as bulla. The fluid inside the bubble can be blood, pus, or serum; which is a clear liquid that protects the skin. In most cases, blisters are not a major health issue, but they can be an indicator of a more serious condition.
Causes of blisters vary. Blisters are commonly caused by wearing poorly fitted shoes that rub against the foot. However, there are many other causes besides from friction; including burns, sunburn, insect bites, frostbite, poison ivy/oak, chemical exposure, impetigo, eczema, viral infections, and more.
Most blisters heal by themselves and do not require immediate medical care. If you have a blister, do not pop it since this may cause infection; it is advised to put a bandage over the blister to protect it. If the blister is large, causes pain, or if you have a fever, it is recommended that you see a doctor who can provide proper care. Blisters are easy to diagnose, and if considered prudent by the doctor, can easily be drained of fluid with a sterile needle as well.
To prevent blisters on the feet, wear shoes that fit properly and don’t cause rubbing. Socks can help prevent friction and it is recommended that you wear them if you are wearing shoes. Hand blisters can be avoided by wearing gloves during activities that cause friction against the hand. If you have a blister that pops, do not remove the dead skin, wash the area, apply antibiotic ointment, and cover with a bandage. It is okay in most cases to not seek immediate medical care for a blister if it was just caused by friction. However, if the blister causes pain or does not go away, it is suggested that you see a doctor for a diagnosis.
Arthritis Can Cause Pain in the Feet and Ankles
Ankle Exercises After a Sprain

Recovering from an ankle sprain requires specific exercises to restore strength, mobility, and stability while reducing the risk of reinjury. Range-of-motion exercises, such as tracing the alphabet with your toes, can help promote gentle movement in the early stages of healing. As the ankle improves, incorporating exercises like the towel stretch can enhance flexibility in the Achilles tendon, which connects the calf muscles to the heel. Ankle strengthening exercises, such as pressing the foot against resistance bands, help rebuild stability in the ankle joint. Balance exercises, including standing on the injured foot, are valuable for improving coordination and preventing future sprains. A podiatrist can assess your ankle sprain, recommend the appropriate exercises, and monitor your recovery to ensure the ankle heals correctly. For severe sprains, surgery may be necessary if other treatments are not effective. If you have sprained your ankle, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and treatment options.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Three Grades of Ankle Sprains
An ankle sprain occurs when one or more ankle ligament gets overly stretched. Ligaments are strong bands of tissue that bind and support the bones and other structures that make up the ankle. In more severe ankle sprains, the ligament(s) tear—either partially or completely—and there may be an audible popping noise at the moment of injury.
Ankle sprains are quite common and can occur when the ankle rolls outwardly (eversion) or inwardly (inversion), causing the ligament(s) to stretch beyond normal limits, or even tear. Falls, twists, or blows to the ankle during sports or other activities can cause this injury, as well as wearing improper footwear, running on uneven surfaces, or having weak ankles.
Depending on the injury’s severity, an ankle sprain will be classified as Grade I, Grade II, or Grade III. Grade I sprains involve ligament(s) being overly stretched but not torn, with symptoms of mild pain, swelling, and ankle instability. There may also be some difficulty bearing weight. A Grade II sprain usually involves a partial tear of the ligament which brings more intensity in these symptoms, along with possible bruising. With a Grade III sprain, the ligament is completely torn, the symptoms are severe, and it may not be possible to put weight on the affected foot at all.
To diagnose and grade an ankle sprain, a podiatrist will perform a physical examination, checking for tenderness and range of motion in the ankle. For more severe sprains, X-rays or other imaging studies may be necessary.
It is vitally important to have an ankle sprain treated properly as improper healing often leads to future ankle sprains and possibly even chronic ankle stability. Treatment for an ankle sprain will vary, depending on its severity, and may include the RICE method (Rest/Ice/Compression/Elevation), physical therapy, bracing, medications, and possibly even surgery to repair a torn ligament. Rehabilitation is very important for the sprain to heal properly and to restore functionality.
Symptoms and Relief for Plantar Fasciitis
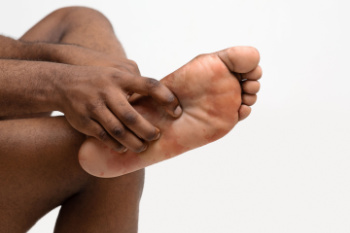
Plantar fasciitis is a condition that results in pain at the bottom of the foot, typically near the heel and arch. This pain often feels like a stabbing or bruising sensation, and may be most intense during the first steps in the morning. For some patients, the discomfort can also occur after standing for long periods of time, or when standing up after sitting for an extended time. Pain from plantar fasciitis may vary in intensity, with severe cases causing significant discomfort during daily activities. Risk factors include having flat feet, high arches, wearing unsupportive footwear, and standing for prolonged periods. Age, specific occupations, and certain pre-existing foot conditions can also contribute to the likelihood of developing plantar fasciitis. A podiatrist can assess your symptoms, identify the underlying causes, and provide effective treatment, such as custom orthotics or other methods to reduce stress on the plantar fascia and alleviate pain. If you have heel pain related to plantar fasciitis, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Foot Pain From Long Walks

Long walks can lead to foot pain due to overuse, wearing improper footwear, or lack of preparation. Common issues include blisters from friction, arch pain from inadequate support, and heel pain caused by plantar fasciitis. Without proper care, these minor discomforts can turn into chronic problems. To prevent pain, wear supportive, well-fitted shoes designed for walking. Use moisture-wicking socks to reduce blisters and consider orthotic insoles for added cushioning and arch support. Stretch your feet and calves before and after walking to maintain flexibility and circulation. If pain persists or worsens, it is suggested that you consult a podiatrist who can identify underlying issues, such as misalignment or overpronation, and recommend tailored solutions like custom orthotics or specific treatments.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
The feet, being the foundation of the body, carry all of the body’s weight and are therefore prone to experiencing pain and discomfort. If you are experiencing foot pain, it is important to determine where in the foot you are experiencing this pain to help discover the cause of it. While pain can be experienced virtually anywhere in the foot, the most common sites of foot pain are in the heel and ankle.
Heel pain can be due to a multitude of conditions including plantar fasciitis, Achilles tendinitis, and heel spurs. Pain experienced in the ankle can be a sign of an ankle sprain, arthritis, gout, ankle instability, ankle fracture, or nerve compression. In more serious cases, pain in the foot can be a sign of improper alignment or an infection.
Foot pain can be accompanied by symptoms including redness, swelling, stiffness and warmth in the affected area. Whether the pain can be described as sharp or dull depends on the foot condition behind it. It is important to visit your local podiatrist if your foot pain and its accompanying symptoms persist and do not improve over time.
Depending on the location and condition of your foot pain, your podiatrist may prescribe certain treatments. These treatments can include but are not limited to prescription or over-the-counter drugs and medications, certain therapies, cortisone injections, or surgery.
If you are experiencing persistent foot pain, it is important to consult with your foot and ankle doctor to determine the cause and location. He or she will then prescribe the best treatment for you. While milder cases of foot pain may respond well to rest and at-home treatments, more serious cases may take some time to fully recover.
What Causes Toenail Fungus?
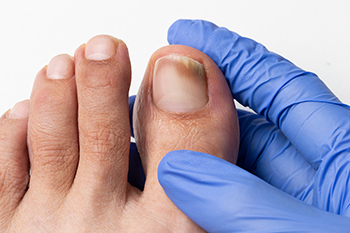
Toenail fungus, also known as onychomycosis, is a common fungal infection that affects the toenails, causing discoloration, thickening, and a crumbly texture. The infection occurs when fungi enter the nail through small cracks or injuries, thriving in warm, damp environments such as sweaty shoes or communal showers. Toenail fungus can also develop when the immune system is weakened or when there is an existing medical condition, such as diabetes, that makes the body more susceptible to infections. The most noticeable symptoms include a yellow or white discoloration of the nail, followed by thickening, brittleness, and sometimes an unpleasant odor. In more severe cases, the nail may separate from the nail bed. To diagnose toenail fungus, a podiatrist will typically examine the affected nail and may take a sample for laboratory testing to identify the specific fungus causing the infection. If you have any of the above symptoms, it is suggested that you contact a podiatrist who can effectively treat toenail fungus, which may include prescribed medication.
For more information about treatment, contact Kenneth Donovan, DPM of Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.