Heel Pain
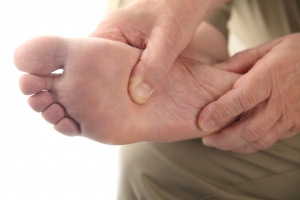
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
The Serious Nature of Diabetic Foot Problems
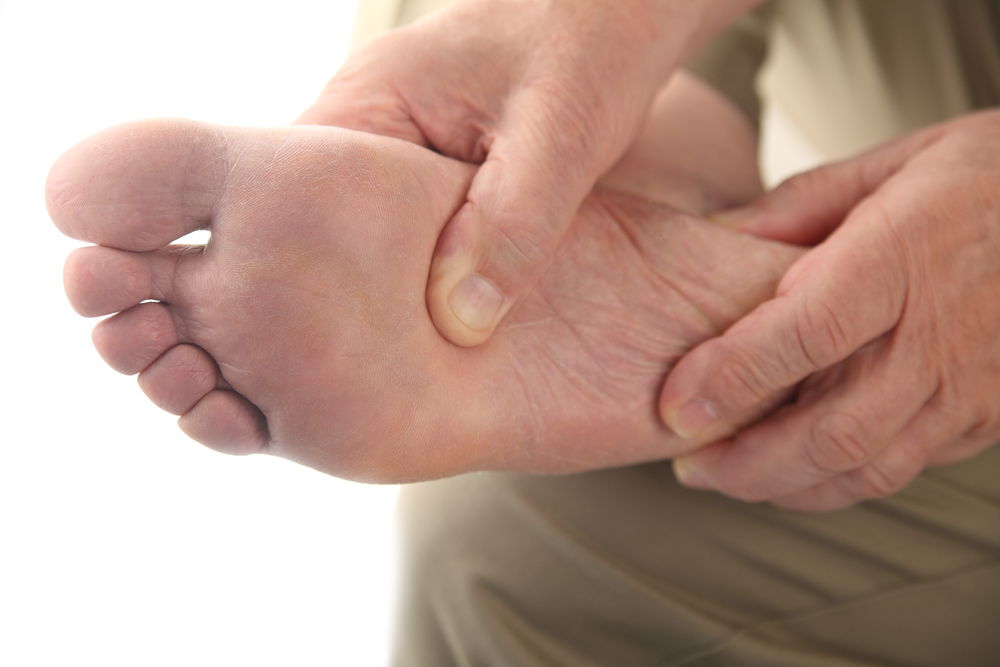
Serious foot infections in diabetic individuals pose significant health risks and often lead to amputations and even death. These infections are a concerning complication of diabetes and require careful attention. They can be caused by various factors, including poor blood sugar control, reduced blood flow, and nerve damage in the feet. In diabetic foot infections, bacteria can enter through minor cuts or sores, leading to cellulitis, abscesses, or even gangrene. Early detection and prompt treatment are crucial to prevent severe complications. Common symptoms include redness, warmth, swelling, and pain in the affected foot. Treatment typically involves antibiotics, wound care, and in some cases, surgical intervention to remove infected tissue and improve blood flow. Diabetic patients must take special precautions to prevent foot infections, such as daily foot inspections, proper hygiene, wearing well-fitting shoes, and maintaining good blood sugar control. If you have diabetes, it is suggested that you schedule regular appointments with a podiatrist to monitor your foot health, and receive timely intervention to prevent serious infections.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetic Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If bone is removed it is then replaced with prostheses, or synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
Definition and Risk Factors of Plantar Warts
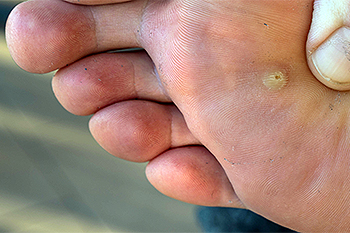
Plantar warts, small growths caused by the human papillomavirus, or HPV, often appear on the soles of the feet. Unlike common warts, which typically grow on the hands, plantar warts can be painful due to the pressure exerted on the soles when walking or standing. These warts may have a rough, grainy appearance with tiny black dots, which are actually clotted blood vessels. Several risk factors increase the likelihood of developing plantar warts. Close contact with the virus, such as walking barefoot in damp and communal areas like locker rooms, swimming pools, or public showers, can put your feet at risk. Additionally, those with a weakened immune system, such as individuals with diabetes or HIV, are more susceptible to plantar warts. Constantly moist or sweaty feet can provide an ideal environment for the virus to thrive. If you have developed a plantar wart, it is strongly suggested that you consult a podiatrist who can provide relief with appropriate treatment methods.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What Are Plantar Warts?
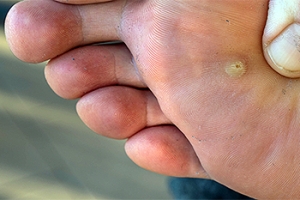
Plantar warts are described as small growths that appear on the heels or other areas of the feet that bear a large amount of weight. The pressure in these areas causes plantar warts to hide behind thick layers of skin called calluses. In most cases, plantar warts are not a serious health issue, and they usually go away without treatment. However, it is still important be mindful of them.
Plantar warts are caused by infections with human papillomavirus (HPV) in the outer layer of skin on the soles of the feet. The plantar warts then develop when the virus enters the body through weak spots at the bottom of the feet, such as tiny cuts and breaks. Plantar warts are not guaranteed for all who encounter the virus. Everyone responds differently to the affects of HPV.
Plantar warts are most common in the following groups: children and teenagers, people with weakened immune systems, people with history of plantar warts, and people who walk barefoot. Exposure to HPV is common in environments such as locker rooms or pool areas.
One of early signs to look out for is a callus, since many plantar warts hide behind them. You can also locate these warts by looking for small, fleshy, rough, grainy growths near the base of the toes and the heel. Early signs of plantar warts are shown by black pinpoints, which are small, clotted blood vessels. Lesions that interrupt normal lines and ridges in the skin of your foot may also be a sign of plantar warts. Any feeling of pain while walking or standing can also be a symptom of plantar warts.
Although most cases are not serious, some conditions may require a visit to your podiatrist. If you are uncertain that your lesion is a wart, if you have diabetes, or if you are experiencing bleeding, you may need to see a seek professional treatment. Your doctor may offer treatments such as prescribing stronger peeling medicine or using cryotherapy by applying liquid nitrogen to the wart. More serious cases may require minor surgery or laser treatment.
There are simple solutions available to help prevent plantar warts. One common task is to avoid walking barefoot in swimming pool areas and locker rooms, as this is where HPV is commonly present. Keeping your feet clean and dry, while changing shoes and socks daily can also help prevent future plantar warts. If you know someone who has plantar warts, it is important to avoid direct contact with their warts. You should also refrain from picking or scratching your wart if you happen to develop one.
Morton’s Toe Can Cause Pain
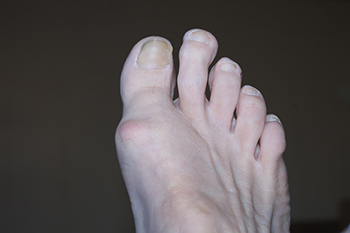
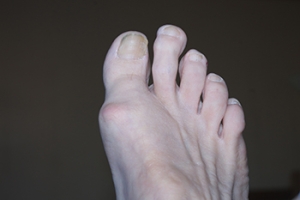
Morton's toe is characterized by the second toe appearing to be longer than the big toe. It is a prevalent foot structure that affects weight distribution and occasionally causes discomfort. Morton’s toe is a hereditary trait that has also been associated with potential advantages in athletics, as many professional athletes exhibit Morton's toe. Morton's toe is not actually caused by the second toe itself. In fact, its root lies in the metatarsals. When the first metatarsal is shorter, it makes the second toe seem longer. This condition leads to uneven weight distribution across the other bones of the feet. Over time, Morton’s toe may result in aches and pains, primarily felt at the base of the first two metatarsal bones and at the head of the second metatarsal. Fortunately, conservative treatments, such as padding, specific exercises, medication, and wearing custom orthotics can effectively manage the associated pain. For cases where conservative measures fall short, surgical options that call for removing certain toe joints are available. Seeking early intervention and consulting with a podiatrist can guide individuals with Morton's toe toward an appropriate and personalized course of action to maintain foot health and overall well being. For more information on Morton’s toe, it is suggested that you make an appointment with a podiatrist.
If you have any concerns about your feet, contact Kenneth Donovan, DPM from Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Biomechanics in Podiatry
Podiatry is a branch of medicine that deals with the study, diagnosis, and treatment of foot and ankle conditions. There are various subdivisions in podiatry; biomechanics is one of them. Biomechanics is the way in which the bones, muscles, and joints of the feet and lower limb interact with each other.
Our feet play crucial roles in the way we move, and it is rare to have feet that are completely symmetrical. Common biomechanical issues include high or low arches or uneven leg heights. Excessive pronation often leads to fallen arches, or flat feet, and is a common cause of running injuries. People whose feet are over-pronated tend to have flexible and unstable feet. Pain is usually experienced during walking and running.
At times, people may be able to adapt to these abnormalities without any difficulties, but in other cases, these issues can cause a great deal of pain. This pain occurs because the joints, muscles, ligaments, and tendons are put under an excess amount of stress during movement. Common symptoms of biomechanical problems stemming from the feet include hip pain, knee pain, leg cramps, ankle pain, lower back pain, weak ankles, tripping, heel pain, Achilles pain, and shin splints.
Many biomechanical issues can be treated with orthotics. Orthotics are shoe insoles that are used to help control the way the foot operates. They can provide relief from foot pain, heel pain, and knee pain. Depending on your specific case, you may need to purchase over-the-counter orthotics or custom orthotics to fit your feet. Your podiatrist will be able to prescribe the perfect orthotic for your feet to help you walk around with ease.
Gait is defined as the way we move our bodies from one point to another. This is usually done by either walking or running. Gait analysis is a method used to assess the way we walk or run to highlight biomechanical abnormalities. Gait analyses are a great way to take a detailed look at how you walk and how your foot moves while you walk. An examination of the feet will help your podiatrist understand why you are suffering pain in other parts of your body.
Birth Defects Impacting a Baby’s Feet

Birth defects affecting the feet can have a significant impact on a child's life. These abnormalities can range from clubfoot, where the foot is twisted inward, to webbed toes or missing toes, irregularly shaped feet, or fused joints. Addressing these issues early is vital for the child's long-term mobility and comfort. Seeing a podiatrist is essential in such cases. Podiatrists are foot specialists who can diagnose and provide early interventions to manage such birth defects. They assess the child's condition, create a tailored treatment plan, and monitor progress. If you have an infant that has been born with a foot deformity, it is strongly suggested that you visit a podiatrist as quickly as possible for an evaluation and treatment plan.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact Kenneth Donovan, DPM of Advanced Care Foot and Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions please feel free to contact our office located in Charleston, SC . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Congenital Foot Problems
A congenital foot problem is a problem affecting the feet, toes, and/or ankle that a child is born with. Several issues with a child’s feet can occur congenitally. Such problems include clubfoot, vertical talus, tarsal coalition, polydactyly, macrodactyly, and cleft foot. Some of these problems have a genetic basis, with someone in their family history having a gene causing the condition, and some are simply an anomaly.
The following are specifics about a few of these conditions:
- Clubfoot, also called congenital talipes equinovarus or talipes equinovarus, is When the tendons of the foot shorten, the bones are of an unusual shape, and the Achilles tendon is tight, causing an inward and downward pointing of the foot. The soles of the feet might also face each other. In most cases of clubfoot, both feet are affected. If not treated, the affected child will walk on the sides of their feet or ankles.
- Polydactyly is a condition where the child has more than five fingers or toes on either or both feet. Presentation usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus is where the talus bone forms in the wrong position, other bones in the foot do not line up properly, the front of the foot points up, and the bottom of the foot is stiff, has no arch, and usually curves out. This can occur in one or both feet and if left untreated, can lead to serious disability or discomfort as the child grows.
- Tarsal coalition is when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot. The tarsal bones, located toward the back of the foot and in the heel, are the ones affected. This condition is often present at birth, but signs of the disorder usually come on in early adolescence.
- Cleft foot is a rare condition where the foot has missing toes, a V-shaped cleft, and other anatomical differences. Surgery can often help improve the foot’s function since the heel remains normal and is what is most needed for walking. The main issues with this affliction are whether the affected foot can fit into a shoe and the shape and appearance of the foot.
- Macrodactyly is when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue. Having this condition makes it harder for the child to use the affected foot for certain activities.